Suicide Prevention in Primary Care Resources
Nearly half of individuals who later end their lives by suicide visit a primary care provider in the month before their passing, making these everyday care visits vital opportunities to identify, assess, and care for these patients. Primary care teams and organizations can play a key role in suicide prevention, and the Association of Clinicians for the Underserved’s Suicide Safer Care (SSC) program helps healthcare workers and organizations incorporate evidence-based strategies and micro-interventions in suicide prevention into everyday primary care.
The below repository collects key resources on suicide prevention in primary care, specific considerations for pediatric, geriatric, and other subpopulations, and more. These resources include both ACU’s SSC publications and webinars, as well as those of our partners and broader field. This project was made possible with the generous support of the Centene Corporation.
If you’re interested in further resources or for free technical assistance or trainings, please contact us.
Click on Any Topic to Jump to a Specific Section:
Suicide Prevention in Primary Care
Step By Step: Routine Screenings and Assessment in Primary Care, Care Management, and Referrals
Routine Screenings and Assessment in Primary Care: Action Steps, Training, & Resources
Step 1: Establish a training plan to support all staff in adopting suicide safe communication strategies.
- National Council for Mental Wellbeing’s Mental Health First Aid
- LivingWorks SafeTALK
Step 2: Identify comprehensive screening and assessment tools like the PHQ-9 and C-SSRS.
- Suicide Screening and Assessment (Suicide Prevention Resource Center)
- Screening and Assessing Suicide Risk in Medical Settings: Feasible Strategies for Early Detection (FOCUS)
- Screening for Suicide Risk (Zero Suicide)
 Step 3: Establish a policy to screen all patients over the age of 12 using a standardized screening tool.
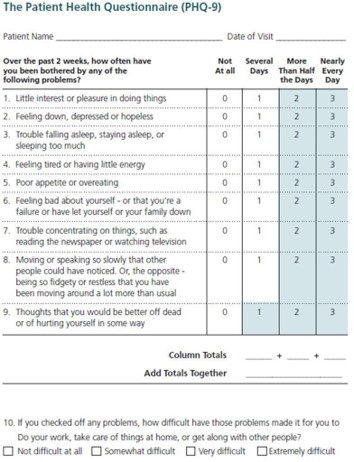
Step 3: Establish a policy to screen all patients over the age of 12 using a standardized screening tool.
- Ask Suicide-Screening Questions Toolkit
- Patient Health Questionnaire – 9 (PHQ-9)
- PHQ-9 Modified for Adolescents (PHQ-A)
- Columbia Suicide Severity Rating Scale
Step 4: Establish protocol for responding to positive depression screens and/or answers of “yes” to question 9 on the PHQ-9.
- PHQ-9: Using PHQ-9 Diagnosis and Score for Initial Treatment Selection (Centers for Health Care Strategies)
- Use of the Patient Health Questionnaire (PHQ-9) in Practice: Interactions Between Patients and Physicians (Qual Health Res.)
- Help Clinic Staff Talk with Patients About the PHQ-9 (AIMS Center)
- Joint Commission Suicide Prevention Portal
Step 5: If possible, update your organization’s EHR to reflect steps outlined in the “Help from your EHR” listings.
- Zero Suicide Toolkit: Engage Individuals at Risk and Implement Suicide Care Management Policies including EHR Monitoring (Zero Suicide)
- Monitoring Suicidal Patients in Primary Care Using Electronic Health Records (J Am Board Fam Med.)
Step 6: Train staff on the protocol for administering the screening and documenting patient responses in the patient record.
- Assessment of Suicidal Risk Using the Columbia Suicide Severity Rating Scale (Zero Suicide)
- Triage and Risk Identification Using the C-SSRS (Columbia Lighthouse Project)
Care Management and Referral Process: Action Steps, Training, & Resources
 Step 1: Review the education materials at Now Matters Now during visits with patients who are at risk of suicide.
Step 1: Review the education materials at Now Matters Now during visits with patients who are at risk of suicide.
Step 2: Train staff and providers on helping at-risk patients make a safety plan.
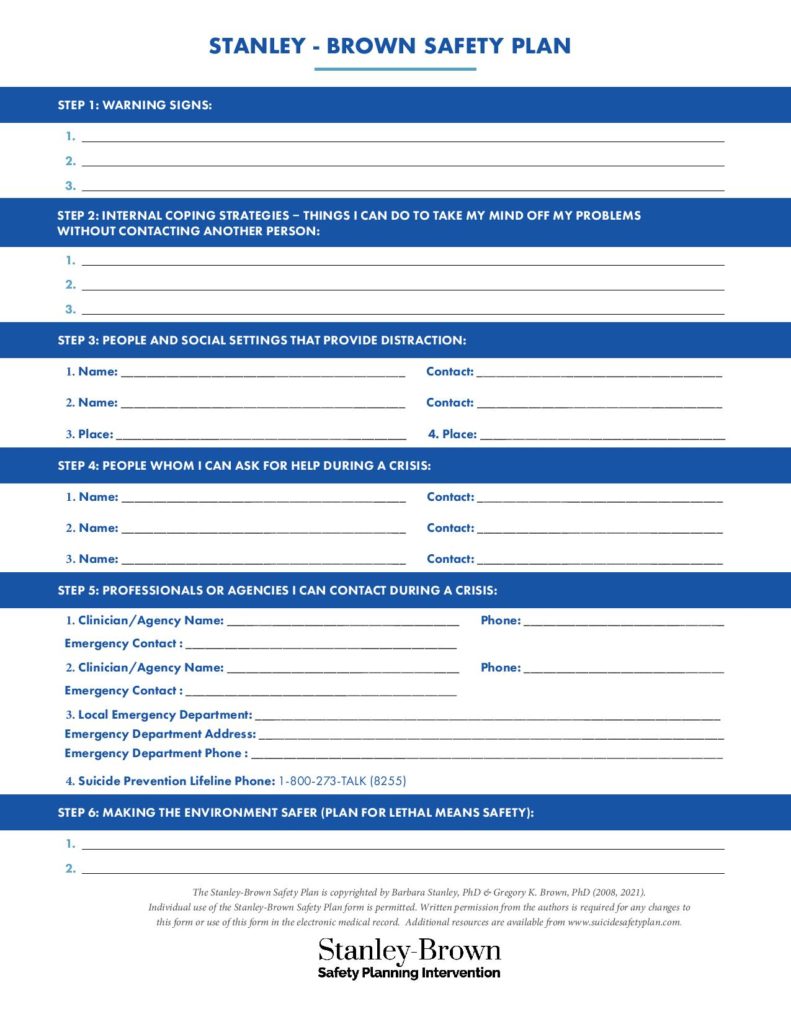
- Stanley-Brown Safety Plan Template (Suicide Prevention Resource Center)
Step 3: Develop organizational policies that clearly state what clinicians and care teams can do to counsel patients on lethal means, including the protocol to follow in the event a patient brings a weapon or other lethal means to the clinical setting.
- Counseling on Access to Lethal Means, or CALM (Zero Suicide)
- Sample Policies and Procedures for Securing Weapons for Suicidal/Homicidal Clients (Zero Suicide)
- Recommendations from the Means Matter Campaign for Clinicians Regarding Guns and Medication (Harvard T.H. Chan School of Public Health)
Step 4: Monitor to ensure that care transitions are documented and flagged for action in an electronic health record.
- Structured Follow-up and Monitoring for Suicidal Individuals (Suicide Prevention Center NY)
- Suicide Care Management Plan (Zero Suicide)
Step 5: Develop internal written policies and procedures, contracts, and memoranda of understanding with outside organizations, including local crisis centers, for safe care transitions.
Publications
Toolkits
Suicide Prevention in Primary Care: A Toolkit for Primary Care Clinicians and Leaders
This publication provides guidance on the four core components of how health care professionals can help identify and prevent suicide in patients, create standards of practice that find suicide unacceptable and set ambitious goals to prevent suicide, and employ evidence-based clinical practices that standardize risk stratification, evidence-based interventions, and patient engagement approaches. Read the guide to learn best practices for screening and identifying and assessing patients at risk for suicide, restricting access to lethal means and safety planning, and caring for patients at risk of suicide.
 Suicide Safer Care: Quick Tips for Medical Students & Other Healthcare Professionals in Training
Suicide Safer Care: Quick Tips for Medical Students & Other Healthcare Professionals in Training
Healthcare professionals in training who will be entering primary care settings are likely to encounter patients at risk for suicide: nearly half of all individuals who end their lives by suicide visit a primary care provider (PCP) in the month before their passing. However, medical students and other clinicians in training often receive little training in prevention. ACU’s “Quick Tips for Medical Students and Other Primary Care Professionals in Training” provides an introduction to elementary suicide prevention strategies that clinicians can integrate in primary care visits. Read the guide to learn how to recognizing warning signs, screen for suicide and assess risk, and intervene.
Brief and Fact Sheet
Excellence in Suicide Prevention in Primary Care & Supporting Healthcare Teams
Suicide is a growing public health crisis in the U.S., affecting both patients and healthcare workers. As essential providers of primary care for 31.5 million patients, health centers have a vital opportunity to identify and treat patients at risk for suicide while simultaneously supporting staff who also may be at risk. ACU’s Centers of Excellence fact sheet and accompanying brief detail key facts and steps in achieving excellence in implementing Suicide Safer Care for patients and staff.
Other Toolkits
- Zero Suicide: Zero Suicide Toolkit
Articles & Research
Selected Research and Documents
- Ahmedani, BK, Simon GE, et al. 2014. “Health Care Contacts in the Year Before Suicide Death.” Journal of General Internal Medicine 29(6): 870-877.
- Luoma JB, Martin CE, and Pearson JL. 2002. “Contact with Mental Health and Primary Care Providers Before Suicide: A Review of the Evidence.” American Journal of Psychiatry 159(6): 909-16.
- McDowell, A, et al. (2011). “Practical Suicide-Risk Management for the Busy Primary Care Physician.” Mayo Clin Proc. 86(8): 792-800.
- Nelson, PA, & Adams, SM. (2020). “Role of Primary Care in Suicide Prevention During the COVID-19 Pandemic.” The Journal for Nurse Practitioners 16(9): 654-659.
- “2012 National Strategy for Suicide Prevention: Goals and Objectives for Action: A Report of the U.S. Surgeon General and of the National Action Alliance for Suicide Prevention.” 2012. Washington, D.C.: US Department of Health and Human Services.
Resource Libraries and Statistics
- Zero Suicide: Evidence Base
- Zero Suicide: Research Articles
- National Institute of Mental Health: Suicide Prevention Resources
- American Foundation for Suicide Prevention: Suicide Statistics
- CDC: Web-Based Injury Statistics Query and Reporting System (WISQARS)
- CDC: Mortality Dashboard
Webinar Recordings
Preventing Suicide in Primary Care for Clinicians & Health Centers
Four-Part Webinar Series | 2024 | Association of Clinicians for the Underserved
 Suicide rates have reached their highest recorded levels in recent years. As vital providers of primary care, community health centers (CHCs) can play a key role in addressing this public health crisis. Half of individuals who end their lives by suicide visit a primary care provider in the month before their passing, making these visits key opportunities to intervene. Reviewed archived sessions in a webinar series from ACU and our primary care association partners to learn evidence-based strategies to identify and intervene with patients at risk, to support clinicians and staff who may themselves be at risk, and to create an environment of Suicide Safer Care for all at CHCs. Sessions in this series include:
Suicide rates have reached their highest recorded levels in recent years. As vital providers of primary care, community health centers (CHCs) can play a key role in addressing this public health crisis. Half of individuals who end their lives by suicide visit a primary care provider in the month before their passing, making these visits key opportunities to intervene. Reviewed archived sessions in a webinar series from ACU and our primary care association partners to learn evidence-based strategies to identify and intervene with patients at risk, to support clinicians and staff who may themselves be at risk, and to create an environment of Suicide Safer Care for all at CHCs. Sessions in this series include:
Clinical Tools and Pathways
Tools for Screening and Assessment
- Patient Health Questionnaire (PHQ-9)
- Patient Health Questionnaire Modified for Adolescents (PHQ-A)
- Ask Suicide-Screening Questions (ASQ) Toolkit
- Columbia Suicide Severity Rating Scale (C-SSRS)
Safety Planning, Lethal Means Restriction, & Micro-Interventions
- Suicide Prevention Resource Center: Stanley-Brown Safety Plan Template
- Now Matters Now: Emotional Fire Safety Plan
- American Journal of Preventive Medicine: “Reducing a Suicidal Person’s Access to Lethal Means of Suicide”
- Dr. Ursula Whiteside: Caring Contacts
Clinical Pathways
- Little, V, & Carbone, T: Sample Suicide Safer Care Clinical Pathway
- Carbone, T, & Little, V: Collaborative Care Management (CoCM) Suicide Safer Care Pathway
- Zero Suicide: Suicide Care Pathway
- Montana Department of Health and Human Services: Clinical Pathway for Patients at Risk for Suicide
Further Resources
Relevant Organizations and Support Services
Pediatric Suicide Prevention
Publications
Toolkit
 Suicide Safer Care: A Toolkit for Pediatric Primary Care Providers and School-Based Health Centers
Suicide Safer Care: A Toolkit for Pediatric Primary Care Providers and School-Based Health Centers
Suicide is the second leading cause of death in youths aged 10-24. However, primary care providers working with pediatric populations at health centers and elsewhere have a crucial opportunity to intervene. Developed in partnership with Concert Health and with the support of the Centene Corporation, “Suicide Safer Care: A Toolkit for Pediatric Primary Care Providers & School-Based Health Centers” provides an overview of pediatric suicide, common risk factors and warning signs, and screening tools, clinical pathways, and evidence-based interventions. Read the publication.
Other Toolkits and Guides
- Little, V., et al. (2024). “A Call to Action for Pediatric Primary Care Providers: Addressing the Rising Suicide Rates Among Children and Adolescents.” Concert Health and Northeast Pediatrics.
- SAMHSA: Evidence-Based Guide: Suicide Prevention Strategies for Underserved Youth
- SAMHSA: National Guidelines for Child and Youth Behavioral Health Crisis Care
- American Academy of Pediatrics: Suicide: Blueprint for Youth Suicide Prevention
- Suicide Prevention Resource Center: It’s Time to Talk About It: A Family Guide for Youth Suicide Prevention
Articles & Research
Selected Research and Documents
- Bridge, JA, et al. (2023). “Youth Suicide During the First Year of the COVID-19 Pandemic.” Pediatrics 151(3).
- Ertl, A, et al. (2020). “Youth Suicide: An Opportunity for Prevention.” Journal of the American Academy of Child & Adolescent Psychiatry 59(9): 1019-1021.
- Shankar, R, et al. (2020). “Youth Suicide: A Population Crying for Help? A System Overloaded? Who Can Help?” Missouri Medicine 117(4): 370-374.
- Shahram, SZ, et al. (2021.) “Promoting ‘Zest for Life:’ A Systematic Literature Review of Resiliency Factors to Prevent Youth Suicide.” Journal of Research on Adolescence 31(1): 4-24.
Resource Libraries
- Zero Suicide: Children and Youth Resources
- NAMI: What You Need to Know About Youth Suicide
- Youth.Gov: Youth Suicide Prevention Resources
Webinar Archives
Pediatric Suicide Prevention for Primary Care Providers and School-Based Health Centers: A Suicide Safer Care Approach
2021 | Association of Clinicians for the Underserved
The crisis of pediatric suicide in the United States is growing. Suicide is the second leading cause of death in youths aged 10-24, with the fastest-growing rates among youth ages 10–14. Furthermore, the crisis is marked by significant racial disparities. However, primary care providers at school-based and other health centers have a crucial opportunity to intervene, and ACU recently developed a new pediatric suicide prevention toolkit for such providers. In this free accompanying webinar, drawing on the new publication and other resources, presenters provided an overview of the crisis and why providers can play an important role in prevention, discussed common warning signs and risk factors, and detailed effective pediatric suicide prevention practices include screening tools such as the PHQ-A and ASQ, as well as clinical pathways and evidence-based interventions.
Clinical Tools and Pathways
Tools for Screening and Assessment
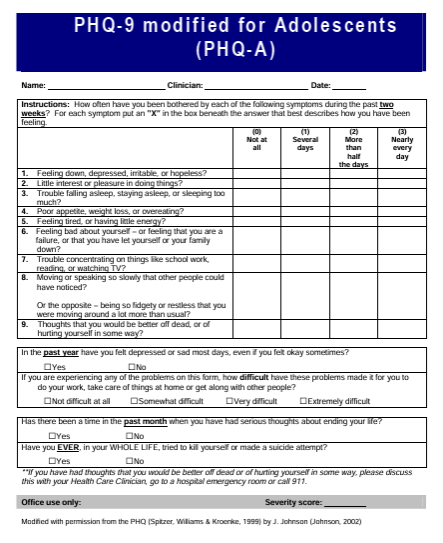 Patient Health Questionnaire Modified for Adolescents (PHQ-A)
Patient Health Questionnaire Modified for Adolescents (PHQ-A)- Ask Suicide-Screening Questions (ASQ) Toolkit
- Youth Ask Suicide Screening Questions (ASQ) Toolkit
- Columbia Suicide Severity Rating Scale (C-SSRS)
Clinical Pathways
- National Institute of Mental Health: Outpatient Youth Suicide Risk Screening Clinical Pathway
- National Institute of Mental Health: COVID-19 Youth Clinical Pathway
Geriatric Suicide Prevention
Publications
Toolkit
 Suicide Safer Care: A Toolkit for Primary Care Providers Working with Geriatric Patients
Suicide Safer Care: A Toolkit for Primary Care Providers Working with Geriatric Patients
Elderly individuals are the greatest risk for completed suicide of all age groups in the United States, and in 2020, 25 people over the age of 65 died by suicide every day. Furthermore, geriatric depression and suicide risk often go under-identified and treated in primary care. Developed by Dr. Virna Little, nationally known suicide prevention expert and Zero Suicide faculty member, ACU’s new “Suicide Safer Care: A Toolkit for Primary Care Providers Working with Geriatric Patients” provides an overview of unique considerations in preventing geriatric suicide, as well as applied strategies that primary care providers working with elderly patients at health centers and elsewhere can utilize. Read the toolkit to learn how to recognize common warning signs, understand risk factors, and incorporate effective geriatric suicide prevention practices and evidence-based interventions.
Fact Sheet
 Geriatric Suicide Prevention and the Role of Primary Care Providers
Geriatric Suicide Prevention and the Role of Primary Care Providers
Developed by Adelphi University’s Dr. Daniel K. Kaplan, an expert on care for geriatric populations, ACU’s new brief explores depression, mental health, and suicide in geriatric populations and how primary care providers and their teams can help. Accompanying our recent webinar on geriatric suicide prevention, this document details the scope of the crisis and provides evidence-based strategies for how primary care teams can help screen for warning signs and address risk of suicide in geriatric patients at health centers and other facilities. Read the brief.
Other Guides
Articles & Research
Selected Research and Documents
- Zilkha, C, et al. (March 4, 2024). “Suicide Rates Are High And Rising Among Older Adults In The US.” Health Affairs Forefront.
- Garnett, MF, et al. (2023). “Suicide Among Adults Age 55 and Older, 2021.” NHCS Data Brief 483 (Nov. 2023).
- McKay, R, et al. (2021). “Toward Zero Suicide for Older Adults: Implications of Healthcare Service Use for Implementation.” Australasian Psychiatry 30(3): 294-297.
- Lapierre, S, et al. (2021). “A Systematic Review of Elderly Suicide Prevention Programs.” Crisis 32(2).
- Conwell, Y, et al. (2011). “Suicide in Older Adults.” Psychiatric Clinics of North America 34(2): 451-468.
- SAMHSA: Suicide Warning Signs and Prevention Strategies for Older Adults
- National Council on Aging: Suicide and Older Adults: What You Should Know
Webinar Recordings
Geriatric Suicide Prevention: Suicide Safer Care Principles for Primary Care Providers and Their Teams
November 2021 | Association of Clinicians for the Underserved
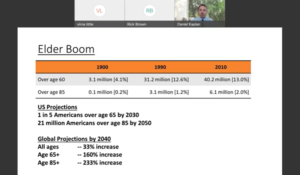 Suicide in elderly populations is a major public health issue. People aged 85 years and older have some of the highest suicide rates of any age group in the U.S., and older adults who attempt suicide are more likely to complete these attempts than others. Additionally, the COVID-19 pandemic has only exacerbated existing risk factors, such as social isolation, depression, and family discord or loss. However, primary care providers and their teams which work with geriatric populations have a critical opportunity to intervene. Learn how Suicide Safer Care principles can help prevent elder suicide in our archived webinar featuring experts from Concert Health and Adelphi University. This discussion explores the dynamics of geriatric depression and suicide and why providers can play important roles in prevention and detail effective suicide prevention practices for geriatric populations, from screening tools to evidence-based interventions.
Suicide in elderly populations is a major public health issue. People aged 85 years and older have some of the highest suicide rates of any age group in the U.S., and older adults who attempt suicide are more likely to complete these attempts than others. Additionally, the COVID-19 pandemic has only exacerbated existing risk factors, such as social isolation, depression, and family discord or loss. However, primary care providers and their teams which work with geriatric populations have a critical opportunity to intervene. Learn how Suicide Safer Care principles can help prevent elder suicide in our archived webinar featuring experts from Concert Health and Adelphi University. This discussion explores the dynamics of geriatric depression and suicide and why providers can play important roles in prevention and detail effective suicide prevention practices for geriatric populations, from screening tools to evidence-based interventions.
View the archived webinar and presentation slides.
How Primary Care Providers Can Help Prevent Elder Suicide: A New Guide to Geriatric Suicide Safer Care
September 2022 | Association of Clinicians for the Underserved
 Elderly individuals are the greatest risk for completed suicide of all age groups in the United States, and in 2020, 25 people over the age of 65 died by suicide every day. Furthermore, geriatric depression and suicide risk often go under-identified and treated in primary care. However, primary care providers working with elderly patients at health centers and elsewhere have vital opportunities to intervene, and the Association of Clinicians for the Underserved has developed a new geriatric suicide prevention toolkit to help. Our webinar with Dr. Virna Little, nationally known suicide prevention expert and Zero Suicide faculty member, provided an understanding of unique factors in geriatric suicide and depression and how providers can act for prevention. Drawing on our publication, the webinar details common warning signs and risk factors, as well as effective geriatric suicide prevention practices and evidence-based interviews.
Elderly individuals are the greatest risk for completed suicide of all age groups in the United States, and in 2020, 25 people over the age of 65 died by suicide every day. Furthermore, geriatric depression and suicide risk often go under-identified and treated in primary care. However, primary care providers working with elderly patients at health centers and elsewhere have vital opportunities to intervene, and the Association of Clinicians for the Underserved has developed a new geriatric suicide prevention toolkit to help. Our webinar with Dr. Virna Little, nationally known suicide prevention expert and Zero Suicide faculty member, provided an understanding of unique factors in geriatric suicide and depression and how providers can act for prevention. Drawing on our publication, the webinar details common warning signs and risk factors, as well as effective geriatric suicide prevention practices and evidence-based interviews.
Further Resources
Relevant Organizations and Support Services
Preventing Clinician Suicide
Publications
Fact Sheet
 Organizational Approaches to Address Suicide Risk in Providers and Staff
Organizational Approaches to Address Suicide Risk in Providers and Staff
Healthcare professionals have significantly higher suicide risk than than individuals in the general population, but many do not seek treatment for fear of stigma or professional repercussions. ACU’s latest publication examines the scope of suicide risk in healthcare professionals and provides organizational approaches to support primary care providers and team members while reducing suicide risk. This fact sheet provides an overview of suicide risk in healthcare team members including physicians, nurse practitioners/physician assistants, and nurses, as well as Suicide Safer Care strategies for managerial training to address suicide risk, approaches to creating environments of wellness, and postvention strategies to support survivors of deaths by suicide. Read the publication.
Toolkit
 Preventing Clinician Suicide & Honoring National Physician Suicide Awareness Day
Preventing Clinician Suicide & Honoring National Physician Suicide Awareness Day
Healthcare professionals are significantly more likely to end their lives by suicide than the general population. Many professionals do not seek treatment or support for fear of stigma or professional repercussions, coping alone with stress, burnout, and fatigue even as they provide care for others. In honor of National Physician Suicide Awareness Day (#NPSADay) on September 17 and year-round, ACU has developed helpful social media resources to help you and your organization raise awareness of the crisis of clinician suicide. Help us raise awareness about the crisis of clinician suicide as well as National Physician Suicide Awareness Day with our toolkit of shareable graphics, messaging, and videos. View the toolkit.
Other Key Resources and Guides
- ACU: Excellence in Suicide Prevention in Primary Care & Supporting Healthcare Teams
- Vital Signs: The Campaign to Prevent Physician Suicide: National Physician Suicide Awareness Day Toolkit
- American Hospital Association: Suicide Prevention: Evidence-Informed Interventions for the Health Care Workforce
- Survivors of Suicide Loss Task Force of the National Action Alliance for Suicide Prevention: Responding to Grief, Trauma, and Distress After a Suicide: U.S. National Guidelines
- Suicide Prevention Resource Center: The Role of Managers in Preventing Suicide
- The National Action Alliance for Suicide Prevention: A Manager’s Guide to Suicide Postvention in the Workplace: 10 Action Steps for Dealing with the Aftermath of Suicide
- Suicide Prevention Resource Center: Comprehensive Blueprint For Workplace Suicide Prevention
Articles & Research
Selected Research and Documents
- Little, V, & Brown, R. (2023). “The Crisis of Clinician Suicide Is Preventable: Organizations Must Take Proactive Steps to Foster Wellness.” Journal of Health Care for the Poor and Underserved 34(4): xii-xvii.
- Barrett, E. (March 2, 2023). “One Way to Stop Stigmatizing Physicians Receiving Mental Health Care.” Institute for Healthcare Improvement.
- Shanafelt, T D, Drybye, L N, et al. (2021). “Suicidal Ideation and Attitudes Regarding Help Seeking in US Physicians Relative to the Working Population.” Mayo Clinic Proceedings 96(8): 2067-2080.
- Kalmoe, M C, Chapman, M B, et al. (2019). “Physician Suicide: A Call to Action.” Missouri Medicine 116(3): 211-216.
- Schwenk, T. L., Davis, L., and Wimsatt, L. A. (2010). “Depression, Stigma, and Suicidal Ideation in Medical Students.” JAMA 304(11): 1181-90.
- Peterson, C., Sussel, A., et al. (2020). “Suicide Rates by Industry and Occupation – National Violent Death Reporting System, 32 States, 2016.” Morbidity and Mortality Weekly Report 69(3): 57-62.
- Davidson, J E, Proudfoot, J, et al. (2020). “A Longitudinal Analysis of Nurse Suicide in the United States (2005-2016) with Recommendations for Action.” WORLDviews on Evidence-Based Nursing: Linking Evidence to Action 17(1): 6-15.
- Rotenstein, L S, Ramos, M A, et al. (2016). “Prevalence of Depression, Depressive Symptoms, and Suicidal Ideation Among Medical Students: A Systematic Review and Meta-Analysis.” JAMA 316(21): 2214-2236.
- Hendin, H., Reynolds, C. et al. (2007). “Licensing and Physician Mental Health: Problems and Possibilities.” Journal of Medical Regulation 93(2): 6-11.
Resource Libraries
- Dr. Lorna Breen Heroes’ Foundation: Learn More
- American Medical Association: Preventing Physician Suicide
- American Foundation for Suicide Prevention: Suicide Prevention for Healthcare Professionals
- American Academy of Family Physicians: Suicide Prevention and Emergency Help
- Zero Suicide: Healthcare Worker Resources
- Suicide Prevention Resource Center: Workplace Resources
Webinar Archives
Caring for the Healers
Five-Part Webinar Series | 2020-Present | Association of Clinicians for the Underserved
 Healthcare workers of many disciplines are significantly more likely to die by suicide than the general population, and many do not seek care for fear of stigma or threats to their professional advancement. Developed by ACU to support the healthcare workforce, the “Caring for the Healers” webinar series explores unique considerations and strategies in preventing suicide among healthcare workers. Featuring a variety of evidence-based practices and subject matter experts, these webinars place a specific emphasis on how organizations and managers can support employee wellbeing:
Healthcare workers of many disciplines are significantly more likely to die by suicide than the general population, and many do not seek care for fear of stigma or threats to their professional advancement. Developed by ACU to support the healthcare workforce, the “Caring for the Healers” webinar series explores unique considerations and strategies in preventing suicide among healthcare workers. Featuring a variety of evidence-based practices and subject matter experts, these webinars place a specific emphasis on how organizations and managers can support employee wellbeing:
-
I: Preventing Suicide Among Providers
-
II: Preventing Suicide Among Providers and Staff
-
III: Preventing Suicide in Healthcare Professionals and Staff and Navigating Postvention
-
IV: Overcoming Barriers and Reducing Stigma to Care for the Healers
-
V: Preventing Suicide in Clinicians and Staff: Holistic Approaches to Caring for the Healers
Informational Videos
Preventing Clinician Suicide: The Scope of the Problem
Watch as Dr. Virna Little, nationally known suicide prevention expert, discusses the crisis of suicide in healthcare professionals and what we can do to help address it and better care for the healers.
Purpose in Practice: Dr. Laura Sidari Shares Her Story of a Mentor’s Death by Suicide
Listen to Dr. Laura Sidari of Cayuga Health as she relates her experience of a physician’s passing and learn why we must ask and take action to help prevent clinician suicide in a short from our Purpose in Practice podcast.






